healthyD Announces Survey Results on Monitoring Habits of Hong Kong Diabetes Patients

healthyD Announces Results on Monitoring Habits of Hong Kong Diabetes Patients Survey
- 90% of Diabetes Patients Fail to Regularly Monitor Blood Glucose Level
- Over Half Have Shortcomings Attributed to Laziness
- Lack of Blood Glucose Monitoring & Control Sharply Induce Risk of Complications
- Patients Expect Accurate Blood Glucose Meter with Alert Function for Better Health Monitoring
[Hong Kong – 12 June 2018] A spreading threat of the world, our world adds a new diabetes patient every three seconds and a new death due to diabetes complications every six seconds, per data from the International Diabetes Federation! Diabetes is a common disease in Hong Kong that about one-tenth of the city’s population is patients! However, majority of diabetes patients neither familiarize with the acceptable standard of blood glucose level nor regularly measure their blood glucose level; along with the absence of systematic blood glucose record, long-term lack of blood glucose monitoring and control also sharply induce risk of complications. In view of this, the Monitoring Habits of HK Diabetes Patients Survey was conducted by healthyD (www.healthyd.com), a health and wellness media platform of ESDlife, from 4 May to 17 May, 2018. Through online questionnaire and questionnaire distribution to diabetes patients followed by the Diabetic Mutual Aid of Hong Kong Association, 421 diabetes patients and 337 family members of diabetes patients were successfully interviewed. By identifying the proficiency of blood glucose level among diabetes patients in Hong Kong, the blood glucose monitoring habits of diabetes patients and their and evaluating the feedbacks among current blood glucose meter users, the survey ultimately aims at underlining the deficiency of existing blood glucose recording method and recommending more effective monitoring method to equip Hong Kong citizens for a better diabetes tackle.
Majority absence of understanding on normal blood glucose level leads to questionable self-monitoring effectiveness
Diabetes patients are required to carry out long-term self-monitoring of blood glucose with blood glucose meter. Among all, diabetes specialists advise special attention on two self-monitoring glycemic indicators: (1) Preprandial capillary plasma glucose refers to the blood glucose measurement made before breakfast and without eating overnight for eight to ten hours. The ideal preprandial glucose goal is within 4.0 – 6.0 mmol/L; (2) Peak postprandial capillary plasma glucose refers to blood glucose measurement made two hours after meal. The ideal peak postprandial glucose goal is no more than 8.0 mmol/L. In the survey, nearly two-fifth of diabetes respondents and family member respondents failed to correctly indicate the ideal preprandial glucose goal, and three-fifth were even unable to correctly indicate the ideal peak postprandial glucose goal. These reflect the reality that even with regular blood glucose measurement, not all diabetes patients can realize whether their blood glucose are at acceptable or alert level without medical professional guidance, causing inappropriate and ineffective blood glucose management among diabetes patients or their family members. According to Dr. Enoch Wu, Specialist in Endocrinology, Diabetes and Metabolism, normal blood glucose level of patients vary with time; besides pre-meal and post-meal differences, age, degree of illness or physique of individuals are factors that affect blood glucose level. Diabetes patients are recommended to consult their doctor to best understand their physical condition, and implement more effective monitoring and control accordingly.
90% of diabetes patients fail to regularly monitor blood glucose level mainly due to laziness
Traditional blood glucose recording requires diabetes patients to follow medical recommendation and jot down the blood glucose measurements on a record book, but there is no standardized format. The survey results found that nearly one-fifth (18%) of diabetes respondents failed to regularly carry out self-monitoring on blood glucose. Even those who said they have a habit of monitoring blood sugar regularly, nearly one-fifth (19%) admitted they did not record their blood glucose levels properly. Among those who claimed they have properly recorded their blood glucose levels, over half (56%) of diabetes respondents said they have been handwriting their blood glucose measurements, while 31% of them jot down the results on white paper. Despite most of the patients tried their best to regular recording their blood glucose measurements, nearly nine-tenth (87%) of diabetes respondents rely on handwritten records that are not standardized and error-prone, creating more difficulties for doctors to follow up. The survey also found a staggering result that 90% of diabetes respondents have forgotten their blood glucose measurements; to specify the reasons for missing the measurement, 55% of diabetes respondent admitted to being lazy, while 34% complained on the inconvenience of handwritten records. As Dr. Wu stated, long-term lack of blood glucose monitoring and control can induce risk of complications. This includes acute complications like hyperglycemia or hypoglycemia, as well as chronic complications such as renal failure, diabetic retinopathy, blindness, diabetes foot, etc. Severe diabetes complication with result in death of heart disease or stroke.
Current imperfections drive patients to expect precise and lightweight blood glucose meter with alert function
For half the century, technology of blood glucose meter has been evolving from time to time. However, 73% of diabetes respondents echo with 84% of interviewed family members that the blood glucose meter they are currently using are not convenient enough and requires improvements. In terms of functional deficiencies on blood glucose meter, there are slight expectation differences between diabetes respondents and interviewed family members. While the former underline blood glucose measurement accuracy (41%) as top priority, the latter primarily address the inclusion of alert function to remind their family members of diabetes patients to take medicines or attend medical follow-up (46%) (See Figure 1). In fact, an app-supported multi-functional smart blood glucose meter with display and alert functions is what diabetes patients and their family members hope to have; this ensures blood glucose records are kept in a more systematic and more convenient way that facilitate doctors to elaborate the readings during follow-up.
Smart blood glucose meter trial by diabetes patients proves more effective measurement management A popular gadget in the world nowadays, global smartphone population is estimated to reach 2.56 billion in 2018. Smartphone penetration rate of Hong Kong now stands at 88.6%; 86% of diabetes respondents and 69% of interviewed family members of this survey are smartphone users. Ironically, only 8% of diabetes respondents and 3% of interviewed family members are using smart blood glucose meter that can be connected with smartphone. Invited by the Diabetic Mutual Aid of Hong Kong Association, Mr. Yuen, a twenty-year sufferer of diabetes, was participated in smart blood glucose meter and mobile app trial. Recording his blood glucose measurement in a handwritten glucose log for years, Mr. Yuen occasionally forgot his blood glucose measurement or somehow felt the process was inconvenient. He hopes he can have a smart blood glucose meter that can conveniently record his blood glucose levels; if there is an app-supported smart blood glucose meter available, he can effortlessly show his blood glucose to the doctor during follow-up for more effective health tracking and blood glucose management.
Appendix
Figure 1: Blood glucose meter expectations between diabetes patients and their family members
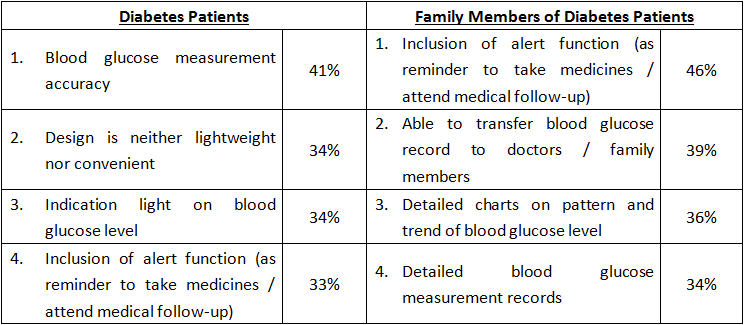
Photo captions


-END-
嘉賓出席「港人衛生意識及皮膚健康調查」結果發布會-1-149x108.jpg)

